Different Levels of Periodontitis
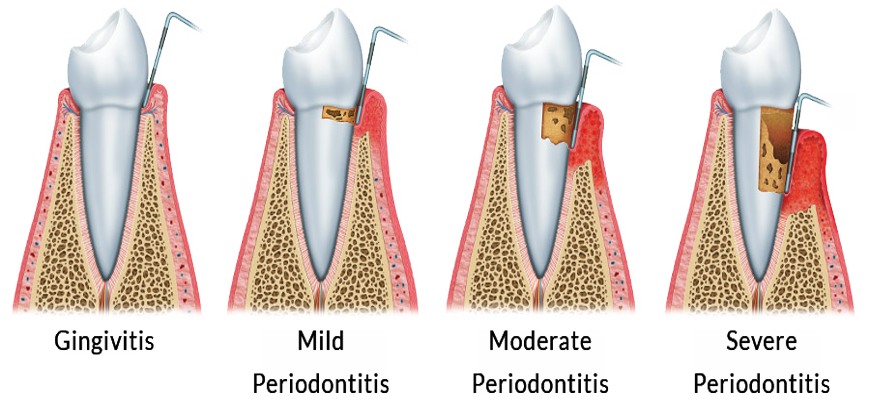
Periodontitis is a term used to describe a group of conditions that involves inflammation of the gums and other structures that support the teeth. Periodontitis is caused by bacteria found in dental plaque and often, but not always, starts as gingivitis.
In trying to eliminate the bacterial infection, your body produces substances that destroy the structures that hold the teeth in the jaw, including the periodontal ligament and underlying bone. As this process continues, the teeth become loose. Pockets form between the teeth and gums, allowing more bacteria to accumulate. Left untreated, periodontitis can result in tooth loss.
Periodontitis usually is relatively painless. The onset of significant pain may signal the development of an abscess.
Older adults are more likely to have periodontitis.
People who smoke are four to seven times more likely than nonsmokers to get periodontitis. Smoking may impair the body’s defense against bacteria.
Causes of gum disease
Gum disease is caused by a build-up of plaque on the teeth. Plaque is a sticky substance that contains bacteria.
Some bacteria in plaque are harmless, but some are harmful for the health of your gums. If you do not remove plaque from your teeth by brushing them, it builds up and irritates your gums.
This can lead to redness with bleeding, swelling and soreness.
Preventing and treating gum disease
Mild cases of gum disease can usually be treated by maintaining a good level of oral hygiene. This includes brushing your teeth at least twice a day and flossing regularly.
You should also make sure you go for regular dental check-ups. In most cases, your dentist or dental hygienist will be able to give your teeth a thorough clean and remove any hardened plaque (tartar).
They’ll also be able to show you how to clean your teeth effectively to help prevent plaque building up in the future. If you have severe gum disease, you’ll usually need to have further medical and dental treatment.
In some cases, surgery may need to be carried out. This will usually be performed by a specialist in gum problems (periodontics).
Different stage classiciation for Periodontitis
Although each procedure varies subtly, there are some basic guidelines to treat cavities, and they are followed by all dental professionals.
-
-
-
-
-
-
-
-
-
-
-
- Mild.
Patients will have probing depths ≤4 mm, CAL ≤1-2 mm, horizontal bone loss, and will require non-surgical treatment. No post-treatment tooth loss is expected, indicating the case has a good prognosis going into maintenance. - Moderate.
Patients will have probing depths ≤5 mm, CAL ≤3-4 mm, horizontal bone loss, and will require non-surgical and surgical treatment. No post-treatment tooth loss is expected, indicating the case has a good prognosis going into maintenance. - Severe.
Patients will have probing depths ≥6 mm, CAL ≥5 mm, and may have vertical bone loss and/or furcation involvement of Class II or III. This will require surgical and possibly regenerative treatments. There is the potential for tooth loss from 0 to 4 teeth. The complexity of implant and/or restorative treatment is increased. The patient may require multi-specialty treatment. The overall case has a fair prognosis going into maintenance. - Very Severe.
Patients will have probing depths ≥6 mm, CAL ≥5 mm, and may have vertical bone loss and/or furcation involvement of Class II or III. Fewer than 20 teeth may be present and there is the potential for tooth loss of 5 or more teeth. Advanced surgical treatment and/or regenerative therapy may be required, including augmentation treatment to facilitate implant therapy. Very complex implant and/or restorative treatment may be needed. The patient will often require multi-specialty treatment.
- Mild.
-
-
-
-
-
-
-
-
-
Good overall oral hygiene and regular checkups can treat and reverse gingivitis. Slight periodontal disease is the second stage of periodontal disease. It is not reversible, but it is manageable. Once a patient reaches stage two, the infection has spread to the bone and begins its bone-destroying process.
The key thing to reversing gum disease is removing the tartar that’s present on both the root of your teeth and under your gum line. Periodontitis can’t be reversed, only slowed down, while gingivitis can be reversed.
Most patients with periodontitis exhibit swollen, dark red, sensitive, or receding gums. Other common symptoms include the development of pus-filled cysts (sacs) in the gum tissue, tooth decay, loose teeth, gaps between the teeth, exposed tooth roots due to gum recession, and tooth loss.
